Pacing
Pacing is a crucial skill to help people break out of the ‘boom and bust cycle’ of behaviour and adopt balanced levels of activity. It is a central feature of becoming more active despite the pain.

What is pacing?
It is common for people with chronic pain to do as much as possible at times when their pain levels are lower. You might hear things like, “I try to catch up on all my jobs before the pain gets me”. They then find the following day they are exhausted, often overwhelmed with pain and unable to do anything at all.
If someone continues to live in this way, they find themselves able to do less and less, even on a ‘good’ day.’
This becomes a vicious and demoralising, self perpetuating cycle often described as ‘boom or bust.’
The alternative is to do nothing and lose fitness. In this case the patient might think, ‘I used to be able to run 10km and I should be able to, but I can’t so it isn’t worth doing any exercise at all.’
In contrast to both these extremes, pacing is about taking a break before pain or tiredness become overwhelming and forces an activity to stop. It is a skill that needs patience and practice. It requires the person to be aware of the effort that an activity involves and balance this with rest breaks or a change in the task.
Ultimately, this can mean that the total amount of activity achieved over a number of days will be greater. This, in turn, helps the person to build up stamina, confidence and self-efficacy.
Your role is to help the person you are working with to understand the concept and techniques of pacing. This is important for retaining their trust as they start to consider changing their activity levels.
Unhelpful pacing patterns
It helps to understand the patterns of activity and rest that people with pain become stuck in. They often prevent them from recovery and improving their quality of life and well-being. Pacing is the second most important skill that people with pain want to change, so supporting people to address this Footstep 3 is really valued.
In a nutshell, there are three unhelpful styles of pacing used by people with pain: overactive, underactive and ‘boom and bust’.
Guiding the person to understand their unhelpful pacing patterns and supporting their changes to a more balanced approach can make a real difference to their range of physical activities and sense of mental well-being and independence.
Overactive pacing
A pattern of doing too much activity or too many tasks over a short space of time.
Pain levels increase and the person often becomes tired quickly. They miss out on the enjoyment of activities, their mood lowers and they have to take time out to recover. Often you find the person has a perfectionist style of thinking and is a completer-finisher. Once they start an activity, a ‘must finish the task’ pattern of thinking dominates. ‘All or nothing’ thinking and activity patterns are unhelpful in recovery and rehabilitation.’
Underactive pacing
Underactive pacing is where the person is doing too little activity or even none. Remaining active is crucial to help maintain stamina and flexibility in muscles, ligaments, joints and bones.
Sometimes in part to help manage their pain and lack of energy/fatigue, a person can spend much of the day resting, sitting or lying down. This contributes to ongoing loss of lack of fitness. Muscles and other tissues become persistently tight or stiff, weak and painful.
This is called deconditioning and can add to the pain experienced. Changing to a more balanced pacing of activities helps improve fitness, mood, sleep and other impacts of pain (see pain cycle).
‘Boom and bust’ pacing
This third pacing pattern is when people using pain and energy levels as a guide to their activities. It means they risk doing too much activity on good days (overactive), which makes pain worse. They then feel forced to rest whilst the pain settles (underactive).
This is a mixed style of pacing and again unhelpful in the long term. It’s sometimes known as ‘boom and bust’ and can be demoralising. This is because as the person tries to become fitter, sleep better and so on, they repeatedly fail, so become depressed, frustrated, etc.
These moods aggravate the pain distress experience and so the pain cycle continues.
The Health and Wellbeing Check is now available online!
Live Well with Pain’s highly regarded tool for assessing the biopsychosocial needs of people with chronic pain can now be accessed right here on this website.
Encourage your patient to do the check and save it as a PDF to share with you at your next consultation.
Explore the new Health and Wellbeing Check here
Or learn how to interpret its results here
Actions to take
Identifying the pacing pattern is a good starting point for action to support self management as there are many things the person can do to develop a more balanced way of carrying out activities.
Your role is to explain about pacing, share suggestions and support pacing skills development so people are more confident they can achieve their own goals.
Pacing is a crucial skill almost every person with pain realises they need – and most are willing to work on this Footstep.
1) Explain the different styles of unhelpful pacing
Understanding the different styles of unhelpful pacing will help the person you are supporting to recognise their own pacing patterns.
2) Help identify tasks that need to be paced
This can be any task that is difficult because of pain, or that can increase pain. It helps to work with the ‘three Ps’:
-
Prioritise – accept it is OK if not everything gets done today
-
Plan the activity itself
-
Pace the activity by speed, distance or duration
Planning is crucial. Talk through how much effort the person can put in without causing their pain to become worse (see effort level scale below).
This will take some trial and error and involves thinking about:
-
Distance of activities
-
Speed of activities
-
Duration of activities
Once the person has identified at what point pain tends to increase, the idea is to put in a break before they reach that point, usually at the half way point.
In persistent pain, people’s pain is present all the time, so it isn’t necessarily helpful to always ‘listen to your body’. However, there is a need for the person to be flexible in their response to pain and activity. Plans may need to be adjusted to take account of day-to-day variations in pain and energy levels and sometimes, other life events may occur which cannot be planned for.
Encourage breaking down activities into smaller tasks or amounts as this helps embed pacing behaviour that leads to success.
For example, washing the car becomes steps of:
-
Preparation, washing the front and bonnet
-
Rest break
-
Washing the back and sides
-
Rest break
3) Emphasise the importance of planning in breaks
For instance, the person could use a timer as a reminder of when to take breaks.
Plan a set rest activity such as having a drink, sitting down and listening to music, doing some breathing exercises.
4) Encourage balanced thinking
Offer strategies to avoid ‘all or nothing’ thinking. For instance, they could:
-
Avoid words like ‘should’ or ‘must’, and replace them with ‘could’
-
Involve friends and family, let them know about pacing and invite support
-
Prioritise – accept it is OK if not everything gets done today
5) Use different approaches to planning activity
The person could divide tasks into different levels of effort: high, moderate and low.
For example:
– Doing all of the ironing, digging the garden for two hours – these involve very high effort levels so better not to do just yet
– vacuuming the downstairs carpets, going for a short bike ride – either of these entail moderate effort, so might be OK to do over next 7-14 days (so long as they are planned and paced well)
– going out to get medicines, seeing a sick family member – these involve low effort, so plan to do these in next 48 hours
Resources you can use with the person you are supporting
Pacing
ALSO AVAILABLE AS A PRINTED BOOKLET
Pacing is a key everyday skill to learn and use for people living with persistent pain. This leaflet offers useful techniques for learning how to balance activities through the day and avoid the common 'boom and bust' cycle experienced by many with persistent pain.

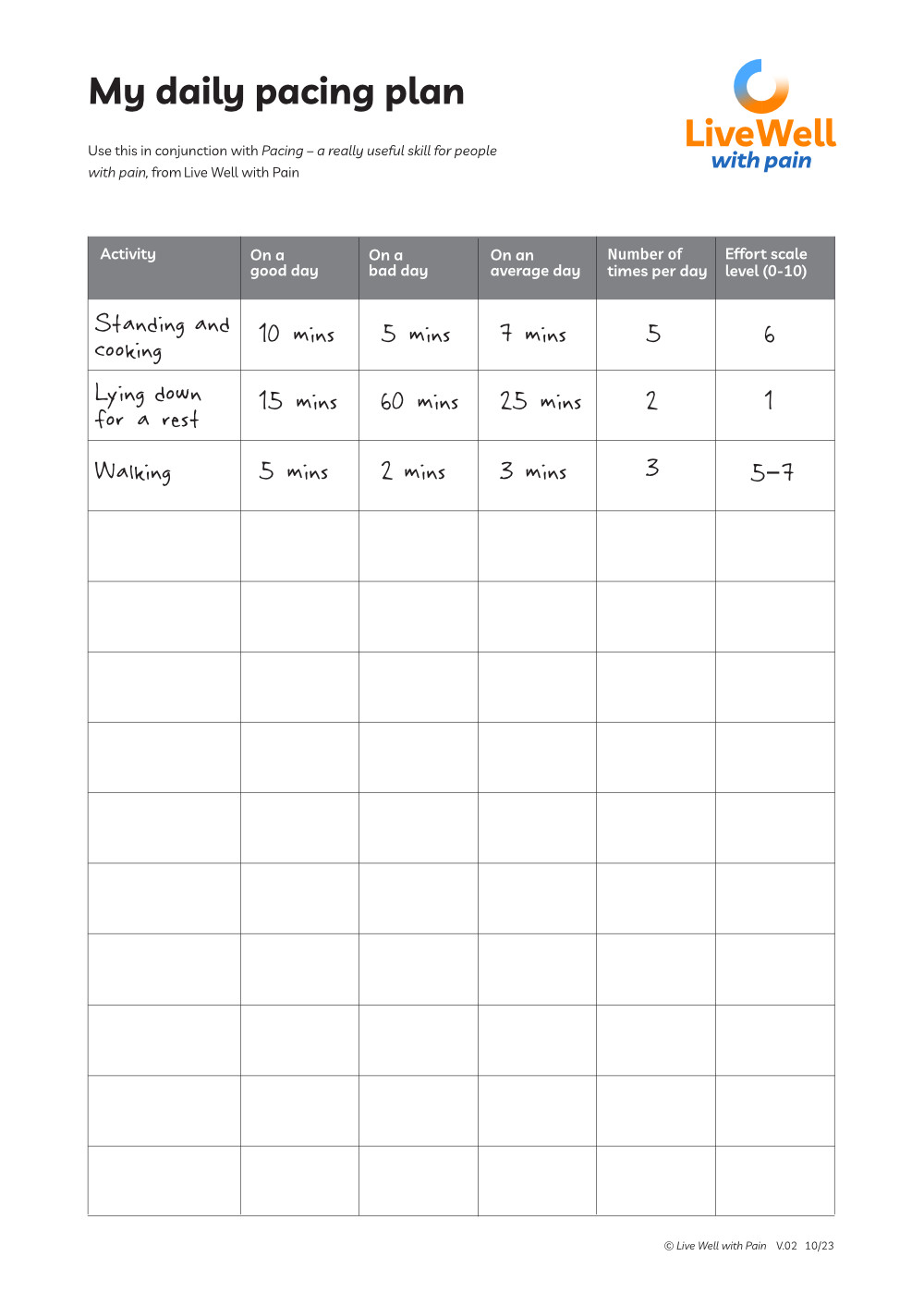
My Daily Pacing Plan
The person you are supporting can create a Daily Pacing Plan to help them balance and pace activities.
The ABC questions can help them build their Daily Pacing Plan:
A: What Activities can I pace today?
B: How long before I take a Break?
C: Check what is the effort level on an Effort Scale
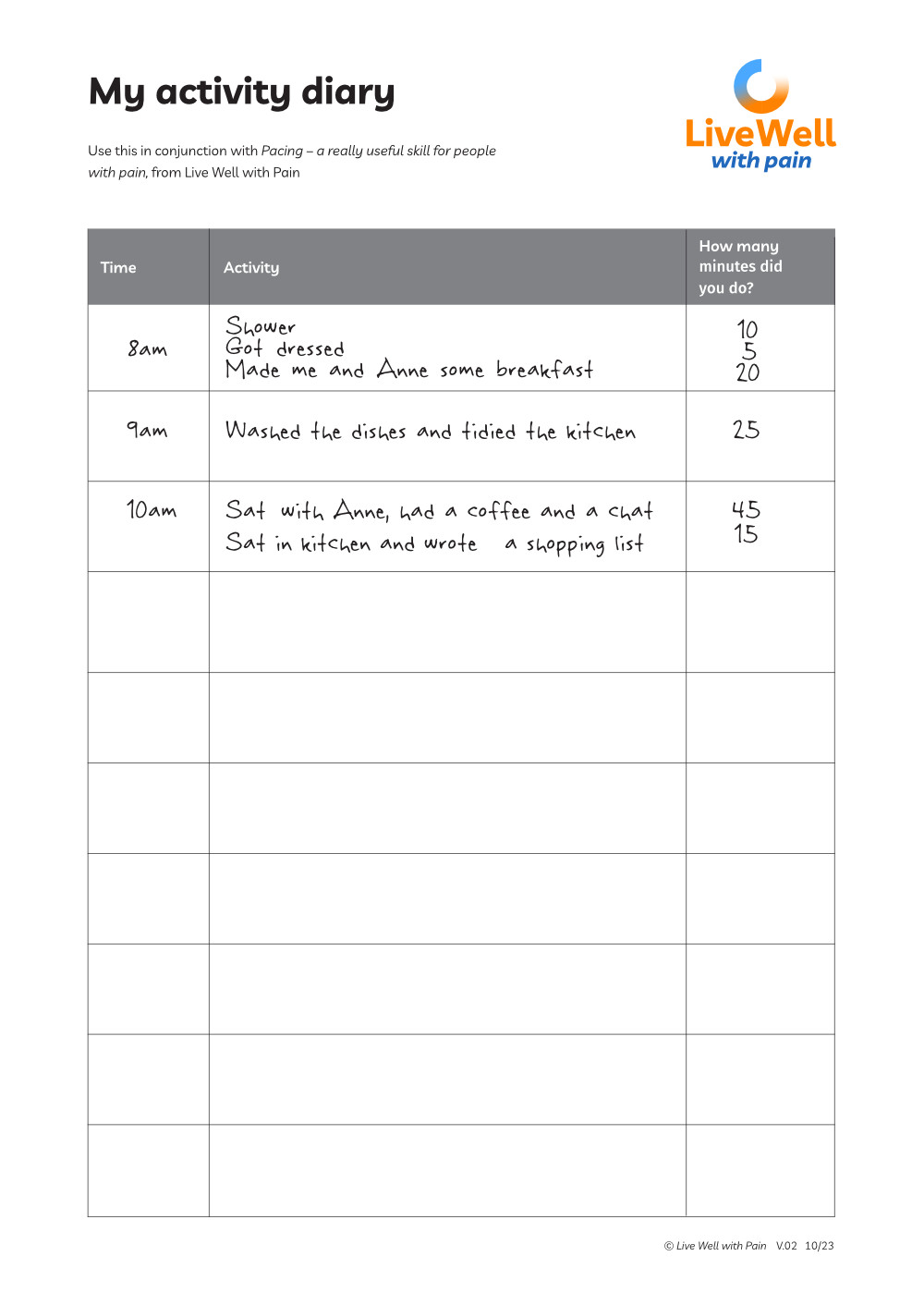
My Activity Diary
This diary or log completed by the person over at least 2-3 days helps them and others understand their current pacing style.
Completing the diary enables a person to track their activities including sleep, rest, sitting or lying down periods, as well as all the activities they carry out through the 24 hours.
It helps to record the minutes spent on each activity to get a fuller picture.
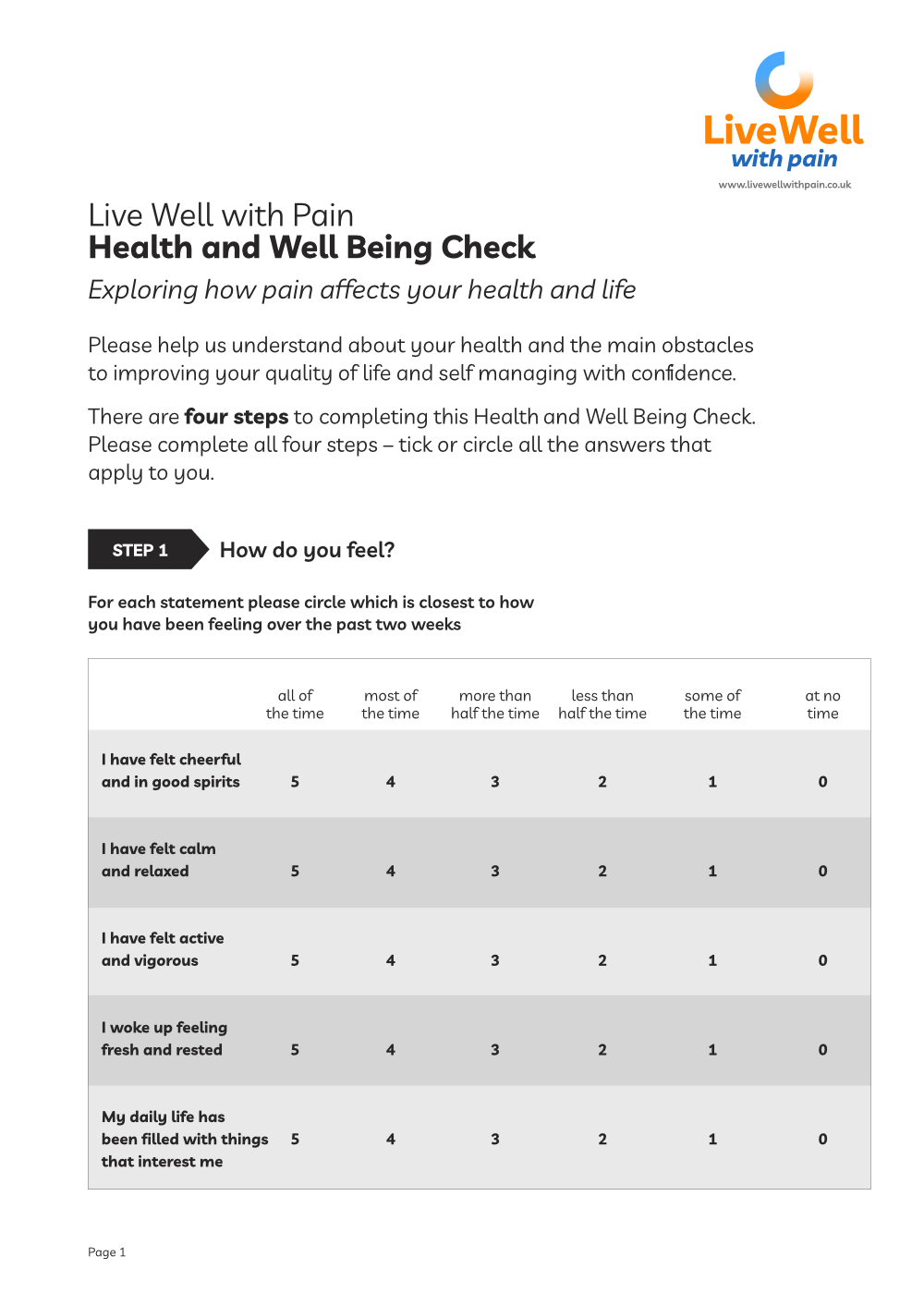
Live Well with Pain Health and Wellbeing Check tool
The Live Well with Pain Health and Wellbeing Check tool is a self-completion, person-centred tool that can be shared easily with patients and clients.
The data from this completed tool will help identify the actual current impact of chronic pain on the individual and their health.
You can find a more detailed explanation of the Live Well with Pain Health and Wellbeing Check tool here.
NEW FOR 2025 – Live Well with Pain's Health and Wellbeing Check is now also online as an interactive tool for people with pain to use. Find it in the resources for people with pain.
Footstep 3 – Pacing
Summary of key points
 Pacing is one of the key self management skills for people living with persistent pain
Pacing is one of the key self management skills for people living with persistent pain
 There are both helpful and unhelpful styles of pacing
There are both helpful and unhelpful styles of pacing
 Unhelpful pacing can lead to setbacks and the person becoming demoralised
Unhelpful pacing can lead to setbacks and the person becoming demoralised
 Helpful pacing can help a person achieve their goals without increasing the pain
Helpful pacing can help a person achieve their goals without increasing the pain
 It is important to discuss pacing before setting goals – especially those goals that are about becoming more active and building strength and stamina
It is important to discuss pacing before setting goals – especially those goals that are about becoming more active and building strength and stamina